Despite being decades old, the Medicare secondary payer rules still cause consternation among group health plan administrators. When does Medicare pay for services, and when does a group health plan foot the bill? The answer depends on two key factors: the size of the group health plan and why the individual is eligible for Medicare.
It's important to understand the difference between Medicare eligibility and entitlement. A person is eligible for Medicare on reaching a certain age or having certain health conditions. A person is entitled to Medicare when he or she is both eligible for Medicare and enrolled in Medicare.
Group Health Plans with 100-Plus Employees
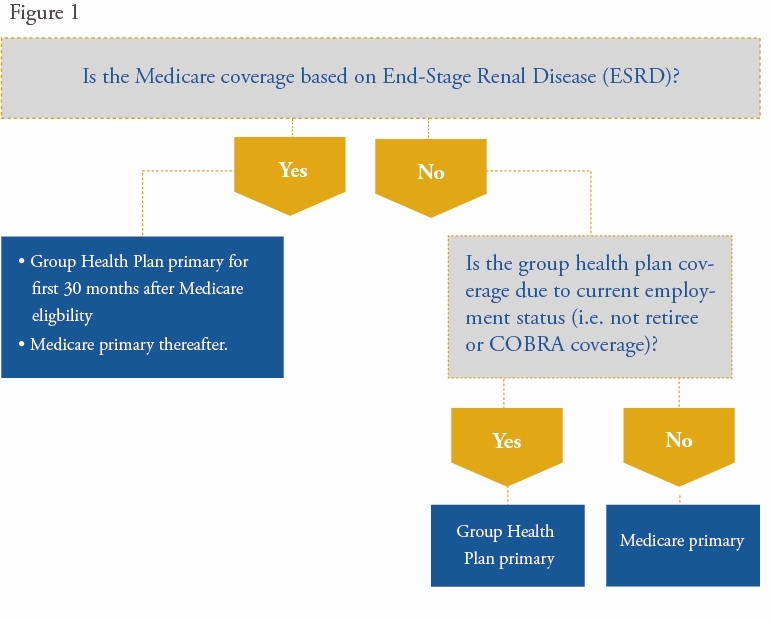
For group health plans with 100 or more employees, the following two-question chart explains whether Medicare or the group health plan is primarily liable for payment:
Group health coverage based on current employment status means that the employee is working or has a continuing business relationship with the employer and that the group health plan covers the employee and dependents because of that relationship.
Current employment status is maintained under many types of paid or unpaid leave. These include Family and Medical Leave Act (FMLA) leaves, Uniformed Services Employment and Reemployment Rights Act (USERRA) leaves, unpaid leaves with an expectation of return, and when the employee is out on disability for the first six months of such leave. Participants do not have coverage based on current employment status when they are covered by retiree plans or through COBRA or severance coverage.
Under the rules, spouses and dependents who are covered by group health plans are considered to have coverage because of the current employment status of the employed family member.
Group Health Plans with Fewer than 100 Employees
Whether Medicare pays first depends on the size of the group and on the reason for the participant’s Medicare eligibility. The following chart explains how Medicare primary coverage depends on employer size:
Medicare Entitlement and Determining Group Health Plan Eligibility
Medicare secondary payer rules prohibit group health plans from taking into account that an individual is entitled to Medicare. This means that group health plans cannot base eligibility or benefits on whether the participant is entitled to Medicare and they cannot charge different premiums or contributions from participants entitled to Medicare.
These rules apply to group health plans that usually are exempted from Employee Retirement Income Security Act (ERISA) rules, such as church and governmental plans. Health flexible spending accounts (FSAs) and health savings accounts (HSAs) are not subject to Medicare secondary payer rules, but health reimbursement arrangements (HRAs) must conform as a group health plan.
Understanding the Medicare secondary payer rules need not be a daunting task. Basically, most plans cannot discriminate in any way against a participant on the basis of the participant’s Medicare entitlement. These rules were put in place so that plans would not take advantage of Medicare by pushing all entitled people and their medical expenses onto the public system.
Ed Doherty is a compliance consultant, health and welfare, at Cammack LaRhette Consulting, which provides health care, HR, employee benefits, retirement, actuarial and communications services.
Was this resource helpful?