PCORI Fee Is Due Aug 2 for Self-Insured Health Plans
For year-end 2020 plans, the fee is $2.66 per enrollee

The annual fee that sponsors of self-insured health plans must pay to fund the federal Patient-Centered Outcomes Research Institute (PCORI) is due Aug. 2, 2021.
The fee applies to health plans for the preceding calendar year. As the IRS announced last year in Notice 2020-84, the current annual fee adjustments are as follows:
- For plan years that ended from Oct. 1, 2020 to Dec. 31, 2020 (including calendar year plans), the fee is $2.66 per person covered by the plan, up from $2.54 a year earlier.
- For plan years that ended last year before Oct. 1, 2020, the fee is $2.54 per person, up from $2.45 the year before.
The Affordable Care Act (ACA) mandated that group health plans pay an annual PCORI fee to fund the Washington, D.C.-based institute, which sponsors research on the comparative effectiveness of medical treatments. The annual fee is usually due July 31, but that falls on a Saturday this year, so the due date is the following Monday.
Although PCORI annual filings and fees were originally set to expire after insurers or employers paid fees in mid-2020 for plan year 2019, Congress reinstated them for an additional 10 years, through 2029, as part of the Bipartisan Budget Act of 2019.
For fully insured group medical plans, insurers report on and pay PCORI fees. For self-funded plans, the employer submits the fee and accompanying paperwork to the IRS.
"Third-party reporting and payment of the fee (for example, by the self-insured plan sponsor's third-party claim payor) is not permitted," wrote Ethan McWilliams, a senior compliance analyst at Lockton, a benefits broker and services firm based in Kansas City, Mo.
Counting Plan Enrollees
Employers can use one of several alternative methods to count the number of plan enrollees, also known as covered lives. The IRS summarizes these methods on its PCORI fee homepage and in PCORI fee FAQs:
- Actual count method. Employers count actual total lives covered on each day of the plan year, add these daily totals together and then divide the total by the number of days in the plan year for average lives covered.
- Snapshot method. Employers take a "snapshot" of average lives covered on one day per quarter. The four quarterly measures are added together and divided by four to get the average.
- Snapshot factor method. Similar to the snapshot method, the number of lives covered on any one day may be determined by counting the actual number of lives covered on that day or by treating those with self-only coverage as one life and those with coverage other than self-only as 2.35 lives. This method likely would not be used for counting health flexible spending account (FSA) and health reimbursement arrangement (HRA) participants, PrimePay software advises.
- Form 5500 method. Employers use a formula that includes the number of plan participants from Form 5500 or Form 5500-SF for the plan year.
When the IRS reinstated the fee in 2020, "plan sponsors were able to use any reasonable method to calculate the average number of covered lives," wrote Karen Hooper, CEBS, a compliance director with the employee benefits division at ABD Insurance & Financial Services Inc. in San Mateo, Calif. This relief "was not extended to the 2021 filing, and employers must use one of the [approved] three methods," she noted.
Making Fee Payments
The IRS views the PCORI fee as an excise tax to be paid midyear. Payment is sent to the IRS with Form 720, which the IRS updated and posted in June.

...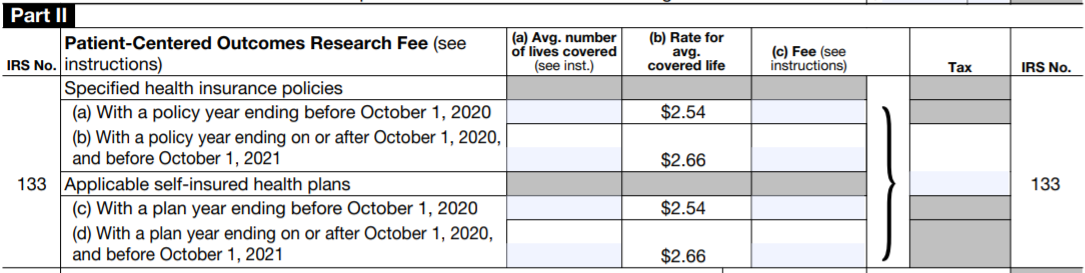
The IRS also revised the Instructions for Form 720.
Payors should remember to check "2nd Quarter" on the Form 720-V payment voucher so their payment is processed properly, McWilliams noted. Failing to do so "will result in the IRS' software generating a tardy filing notice, with all the incumbent aggravation on the employer to correct the matter" with the IRS.
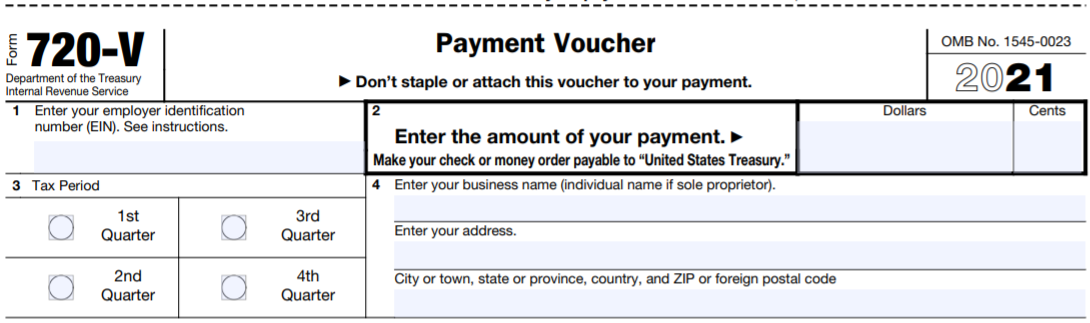
The fee cannot be paid from Employee Retirement Income Security Act (ERISA) plan assets, "except in the case of union-affiliated multiemployer plans," McWilliams explained. The fee also "cannot be paid in whole or part by participant contributions or from a trust holding ERISA plan assets."
PCORI fees, he added, "should not be included in the plan's cost when computing the plan's COBRA premium. The IRS has indicated the fee is, however, a tax-deductible business expense for sponsors of self-funded plans."
FSAs, HRAs and Other Benefits
FSAs and HRAs are considered self-insured health plans subject to the PCORI fee unless they meet one of two exclusions:
- The plan is primarily for employees working or residing outside the U.S.
- The plan is considered an excepted benefit.
Generally, health FSAs are considered excepted benefits and do not require a Form 720 "unless the employer—and not just the employee—makes contributions to it that exceed the lesser of $500 annually or a dollar-for-dollar match of the employee's contribution," said Gary Kushner, president and CEO of Kushner & Company, an HR strategy and employee benefits consulting firm in Portage, Mich. "In that event, those FSAs must also be included in filing the Form 720."
For HRAs, employers should "first look at the integrated group health plan," Kushner advised. "If the [health] plan is fully insured, then the employer must file the 720" and pay the fee for each employee with an employer-funded HRA. The fee is paid per employee, and spouses and children covered by the fully insured health plan are not included in the fee calculation.
"If, however, the underlying group health plan is self-funded, then no separate 720 need be filed for the integrated HRA, but rather, one filing and fee for the self-funded group health plan is due," Kushner noted. In this case, the fee is calculated based on covered lives, not just employees.
The PCORI fee does not apply to health savings account (HSA) participants, as HSAs are individual accounts, not group health plans. It also does not apply to dental and vision coverage that are excepted benefits, and, Hooper noted, "virtually all dental and vision plans are excepted benefits."
Missed Payment Deadlines
"An employer that overlooks reporting and payment of the PCORI fee by its due date," McWilliams wrote, "should immediately, upon realizing the oversight, file Form 720 and pay the fee (or file a corrected Form 720 to report and pay the fee, if the employer timely filed the form for other reasons but neglected to report and pay the PCORI fee)." Employers in this situation should be sure to use the form for the appropriate tax year.
"The IRS might levy interest and penalties for a late filing and payment, but it has the authority to waive penalties for good cause," he noted.
Was this resource helpful?



