Average Worker Paid $5,588 Out of Pocket for Family Health Coverage This Year
Plan deductibles have more than doubled, on average, since 2010

Workers with employer-sponsored health coverage paid 17 percent of the premiums for single coverage this year, on average, and 27 percent of the cost for family coverage, a benchmarking study of nearly 1,800 small and large U.S. employers found.
Annual premiums for employer-sponsored family health coverage reached $21,342 this year, up 4 percent from last year, with workers on average paying $5,588 toward the cost of their coverage and employers paying the remaining $15,754, according to the nonprofit Kaiser Family Foundation (KFF) 2020 Employer Health Benefits Survey, conducted from January to July.
Deductibles Spiked, Then Held Steady
Higher deductibles have become much more common, and the percentage of covered workers with an annual deductible of $2,000 or more for single coverage grew to 26 percent from 19 percent over the past five years, the survey showed.
Eighty-three percent of covered workers had a deductible in their plan this year, similar to last year and up from 70 percent a decade ago. Deductible amounts varied by type of plan. For example:
- The average deductible for single coverage is $1,204 for preferred provider organization (PPO) plans, virtually unchanged from $1,206 in 2019 but up sharply from $675 in 2010.
• For high-deductible health plans (HDHPs), the average single-coverage deductible is $2,303.
- The average deductible for family plans is $2,716 for PPO plans, down slightly from $2,883 last year but up from $1,518 a decade ago.
• For HDHPs, the average family coverage deductible is $4,552.
"The burden of health costs on workers remains high, though not getting dramatically worse," KFF President and CEO Drew Altman said. "Things may look different moving forward as employers grapple with the economic and health upheaval sparked by the pandemic."
Cost-Sharing Amounts
After paying the deductible, most covered workers face a flat-dollar co-payment when they visit a doctor, and some workers face co-insurance requirements—a percentage of the covered amount. KFF's survey showed that this year:
- Average co-payments were $26 for in-network primary care and $42 for specialty care.
- Average co-insurance rates were 18 percent for primary care and 19 percent for specialty care.
These amounts were similar to those in 2019. Out-of-network cost-sharing charges can be significantly higher.
Virtually all covered workers are in plans with a limit on in-network cost-sharing, known as the out-of-pocket maximum. Those limits vary widely. For single coverage, 11 percent of covered workers were in plans with maximums of less than $2,000 and 18 percent of covered workers were in plans with maximums of at least $6,000.
Premiums Outpace Earnings
For 2020, premiums in employer-sponsored health plans rose 4 percent from 2019, the survey found:
- Overall, premiums in employer plans averaged $21,342 for family coverage and $7,470 for individual-only coverage.
- For HDHPs, average annual premiums were somewhat lower—$20,359 for family coverage and $6,890 for individual-only coverage.
The 4 percent premium increase in 2020 was only slightly higher than the year-to-year rise in workers' earnings (3.4 percent) and inflation (2.1 percent). Since 2010, however, average family premiums have increased 55 percent, at least twice as fast as wages (27 percent) and inflation (19 percent), KFF reported.
Employer Premiums and Deductibles Rose Much Faster than Wages Since 2010
Deductibles are for single coverage among insured workers.
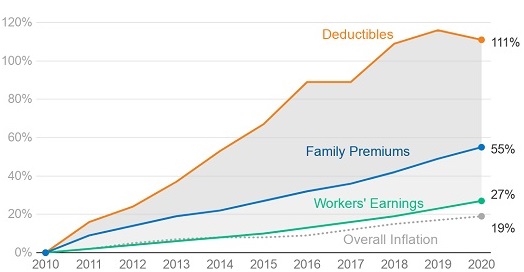
Source: Kaiser Family Foundation.
Although the KFF benchmarking survey did not ask about premium increases for 2021, other studies show that employers expect moderate health plan cost increases next year, primarily in the range of 4.4 percent to 5.3 percent, on average.
Narrow Mental Health Networks
A large majority (83 percent) of employers were satisfied with the overall choice of doctors and hospitals available through their insurance plans, though significantly fewer (67 percent) said the same about their mental health and substance abuse networks, KFF reported
About 1 in 5 (19 percent) describe their mental health networks as somewhat or very narrow, potentially leaving workers with limited options at a time when worry and stress related to the pandemic are affecting many working Americans.
"The coronavirus pandemic has increased the need for access to mental and behavioral health services, for which the provider networks are often more narrow than for other services," said Gary Claxton, a KFF senior vice president and the lead author of the study. "Some plans have been able to increase access by supporting telehealth, though it's unclear whether such options will become a permanent feature."
"The COVID-19 pandemic has created significant mental health challenges for many around the world," Milliman, a global consulting and actuarial firm, similarly reported. "Telehealth visits may become part of the new 'normal' for replacing, or at least supplementing, office-visit-based treatment for behavioral health conditions."
Related SHRM Articles:
Moderate Cost Increases Projected for Health Benefits in 2021, SHRM Online, October 2020
Biden and Trump Want Lower Health Care Costs, but Approaches Differ, SHRM Online, September 2020
Employers Project Health Plan Costs Will Rise 5.3% for 2021, SHRM Online, August 2020
15 Ways Employers Can Reduce Health Care Spending That Aren't Cost-Sharing, SHRM Online, February 2019
Was this resource helpful?



