Employers Project Health Plan Costs Will Rise 5.3% for 2021
Costs per worker, including premiums and out-of-pocket spending, could hit $15,500

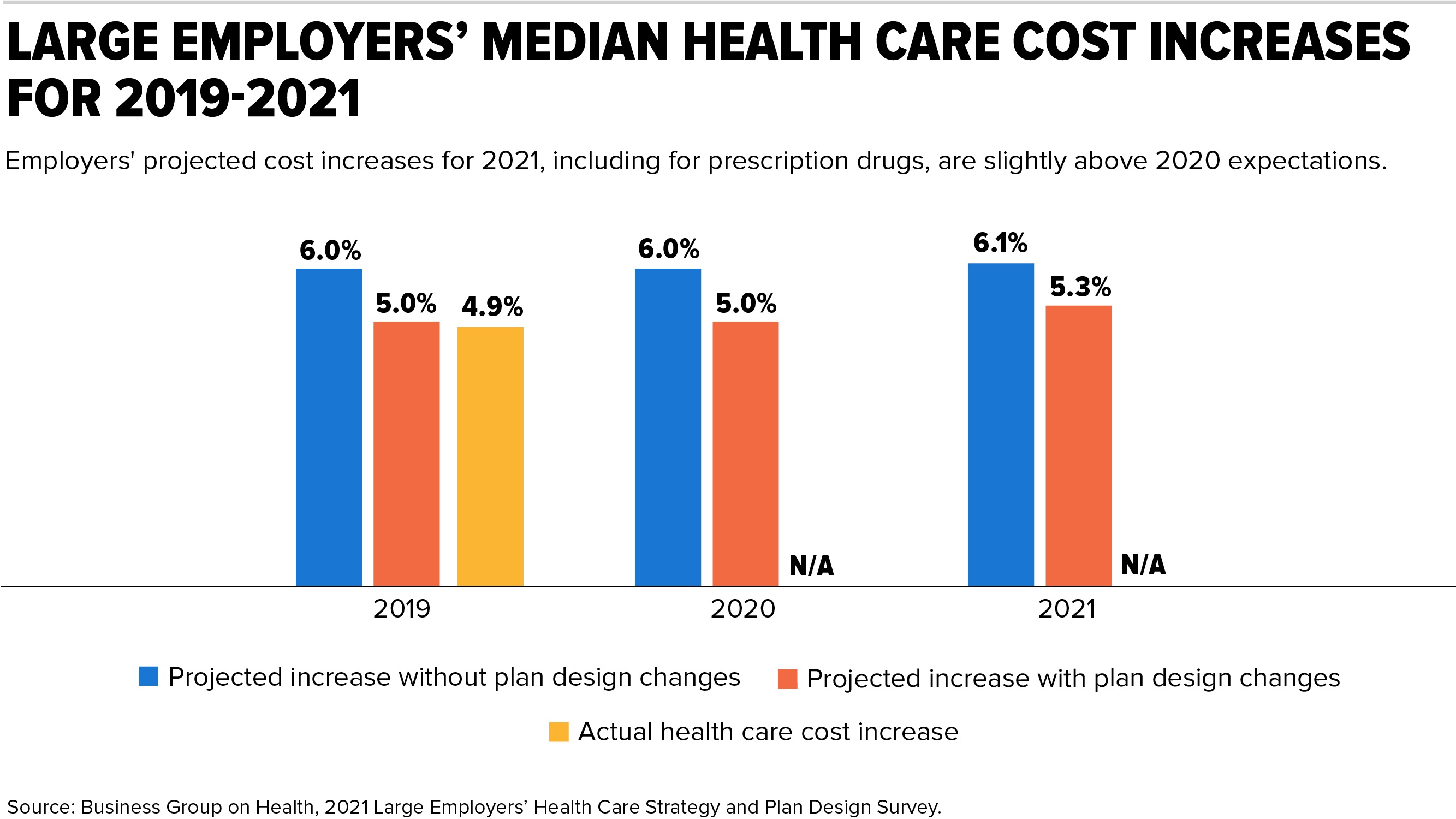
Large employers project that their health benefits costs will rise 5.3 percent in 2021, although the COVID-19 pandemic is fueling uncertainty about overall expenses, a new survey of large U.S. employers shows.
The projected rise in health benefits costs, which takes employers' health plan cost-management changes into account, is slightly higher than the 5 percent increases large employers projected in each of the last five years, according to newly released results from an annual survey by the nonprofit Business Group on Health (BGH), which represents large employers.
The group's 2021 Large Employers' Health Care Strategy and Plan Design Survey was conducted in May and June 2020, and it captured responses from 122 large employers offering coverage to more than 9.2 million employees and dependents. Seventy-seven percent of respondents each have more than 10,000 employees.
Employer and Employee Costs
Including premiums and employees' out-of-pocket costs, average total health care spending is estimated to reach $14,769 per employee this year, up $197 from 2019. Total costs are projected to rise to an average of just over $15,500 in 2021.
The survey further showed that in line with recent years, large employers will cover nearly 70 percent of costs while employees bear about 30 percent:
- For 2020, that leaves employers paying about $10,340 per covered employer or dependent, with employees paying about $4,430.
- For 2021, those amounts are expected to reach about $10,850 and $4,650, respectively.
"Health care costs are a moving target and one that employers continue to keep a close eye on," said Ellen Kelsay, BGH's president and CEO. "The pandemic has triggered delays in both preventive and elective care, which could mean the projected [cost] trend for this year may turn out to be too high. If care returns to normal levels in 2021, the projected trend for next year may prove to be too low. It's difficult to know where cost increases will land," which will require employers to be flexible with health care budget revisions in the coming year.
The 5 Most Costly Conditions 2020 is no different from 2019 when it comes to the top five conditions driving health care costs. For both years, employers ranked those conditions as follows: 1. Musculoskeletal issues such as lower-back pain and knee and hip replacements. 2. Cancer. 3. Cardiovascular (heart) disease. 4. Diabetes. 5. High-risk maternity/neonatal intensive care. |
[SHRM members-only toolkit: Managing Health Care Costs]
Virtual Care Growth
There's no question that use of telehealth services rose sharply during the pandemic. "While employers have been implementing more virtual solutions in recent years, the pandemic caused the pace to accelerate at an astronomical rate," Kelsay said.
Among respondents, 76 percent made changes to provide better access to telehealth services, and 71 percent increased the number of telehealth offerings, such as by adding health coaching and emotional well-being support.
Tellingly, 80 percent of respondents believe virtual health will play a significant role in how care is delivered in the future—a sharp increase from 64 percent last year and 52 percent in 2018.
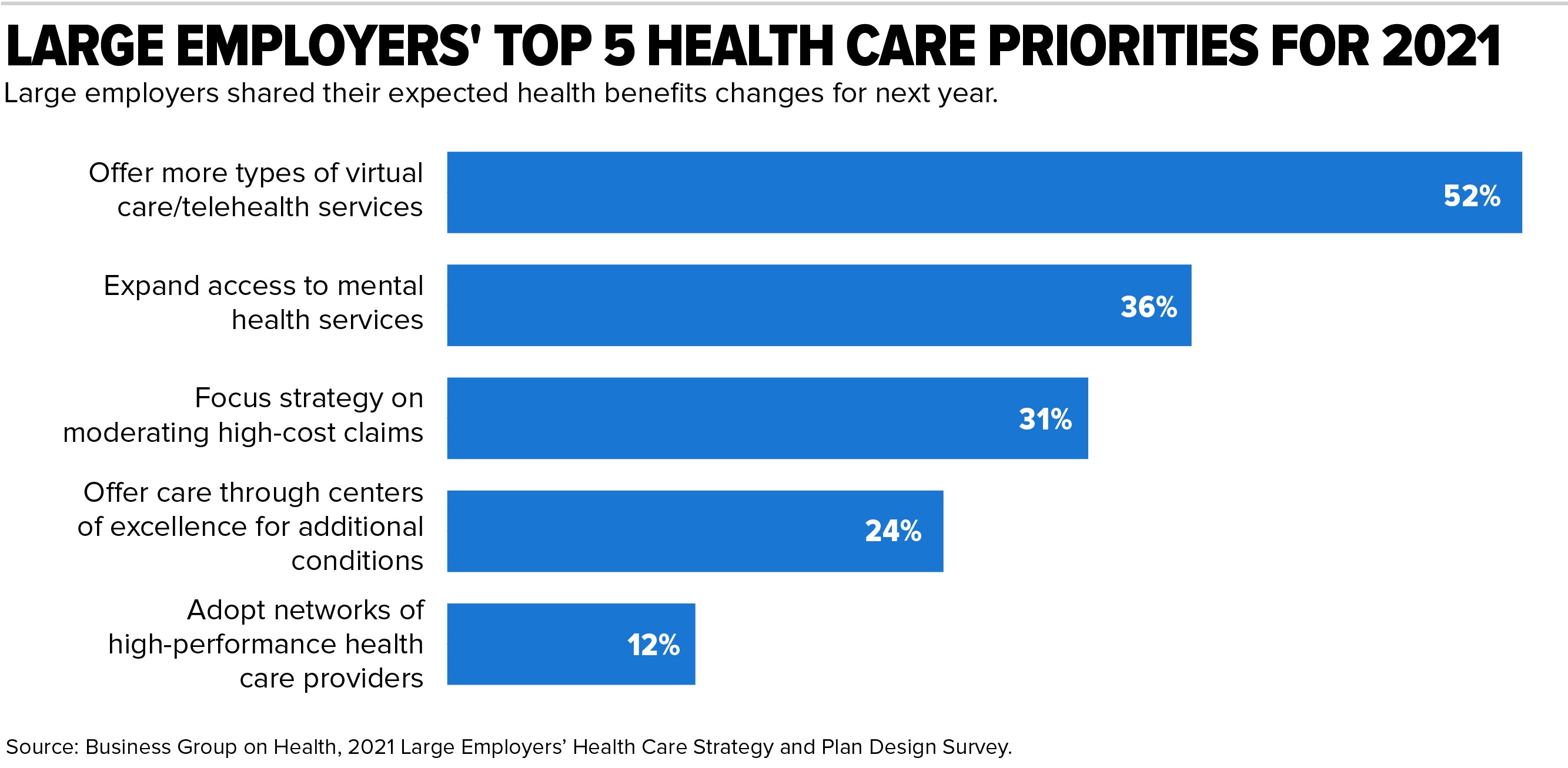
Among other telehealth trends, the survey showed:
- More than half of respondents (52 percent) will offer more virtual care options next year.
- Nearly all will offer telehealth services for minor, acute services.
- While 91 percent will offer telemental health (online counseling or therapy), 96 percent said they will offer telemental health services by 2023.
- Virtual care for musculoskeletal issues, such as physical therapy for back and joint pain, shows the greatest potential for growth. While 29 percent will offer musculoskeletal management virtually next year, another 39 percent are considering adding it by 2023.
Self-Insured Employers Saved as Elective Procedures Declined "People are holding off on elective surgeries and routine care in response to the pandemic," wrote Keith Lemer, CEO of WellNet Healthcare, a health care management and advisory firm for employer-sponsored benefits. "The decline in elective procedures has paid off for… organizations that self-insure, or cover their employees' health costs directly," he noted. Fully insured employers haven't seen cost savings this year from the falloff in non-pandemic health care, although insurance companies have profited because "insurers don't have to pay for care that patients forego." Still unknown, however, is whether there will be a surge in health care use, including delayed elective procedures, into 2021 as the pandemic wanes. |
Mental Health and Well-Being
Another key trend for employer plans in 2021 is the expansion of access to virtual mental health and emotional well-being services, which can reduce the stigma associated with seeking care.
More than two-thirds of respondents (69 percent) provide access to online mental health support resources, such as apps, videos and articles, and that number is expected to jump to 88 percent in 2021.
Employers are also taking other steps to bolster mental health services:
- Roughly half (47 percent) provide manager training on recognizing mental and behavioral health issues and directing employees to services. Another 18 percent plan to do so in 2021.
- Half of respondents (50 percent) will conduct campaigns against stigmatizing those dealing with mental health challenges in 2021.
Large employers are also helping to address cost barriers by reducing out-of-pocket costs for mental health services:
- More than half (54 percent) are lowering or waiving costs for virtual mental health services in 2021.
- More than a quarter (27 percent) will reduce the cost of counseling services at the worksite, bolstering the trend of bringing services directly to employees.
"Employers were already prioritizing mental health and emotional well-being before the pandemic hit," Kelsay said. "Many more employees and family members are now dealing with anxiety, stress or loneliness. We expect employers will boost their investment in programs that support employees' mental health and emotional well-being."
New Approaches
Employers also are thinking strategically about health care, and more are considering actions such as the following:
- Linking health care with workforce strategy. The number of employers that view their health care strategy as an integral part of their workforce strategy increased to 45 percent this year from 36 percent in 2019.
- Focusing on primary care. Over half of respondents (51 percent) will have at least one advanced primary care strategy next year, up from 46 percent in 2020. Supporters of these arrangements say contracting directly with primary care providers can improve the delivery of preventive services, chronic disease management, mental health and whole-person care.
- Addressing high-cost drug therapies. Two-thirds of respondents (67 percent) cited the effect of new million-dollar treatments as their top pharmacy benefits management concern.
Cautious Outlooks for 2021 Consultancy PwC's Health Research Institute recently projected that medical cost increases for employer-sponsored health plans would fall in the 4 percent to 10 percent range. "For the first time in the 15-year history of our medical cost trend report, we did not come out with a single number for the growth rate" in the upcoming year, said Ben Isgur, leader at the Health Research Institute. The reason for that outcome, he explained, was the number of unknown variables related to the use of health care services due to the pandemic. Michael Thompson, president and CEO of the National Alliance of Healthcare Purchaser Coalitions, sees another sign of caution: He doubts that employers will be making drastic changes to their health plans for 2021. "Employers have been terribly distracted by trying to get back to business, to get people back into the workplace, and managing through the [COVID-19] crisis," he said. "All the strategic planning that normally would happen around this time of the year has been put on hold." By the end of 2021, however, Thompson expects employers will be acting on health care lessons they've learned during the pandemic. "We could have radical changes in employer [health benefits] strategy coming out of this," he said, "but I don't think we're going to be looking at it" for the 2021 plan year. |
Related SHRM Articles:
Moderate Cost Increases Projected for Health Benefits in 2021, SHRM Online, October 2020
Well-Being Programs, Voluntary Benefits Help Stressed Employees Cope, SHRM Online, July 2020
IRS Proposes Letting HRAs Pay Direct Primary Care and Health Ministry Fees, SHRM Online, June 2020
Mental Health Apps Offer New Ways to Support Employees, SHRM Online, May 2020
Virtual Physical Therapy Could Be Telehealth's Sweet Spot, SHRM Online, November 2019
15 Ways Employers Can Reduce Health Care Spending That Aren't Cost-Sharing, SHRM Online, February 2019
Was this resource helpful?



