Managing High-Cost Claimants Is Employers' Top Health Savings Strategy
Helping employees with chronic conditions to stay healthy can pay dividends

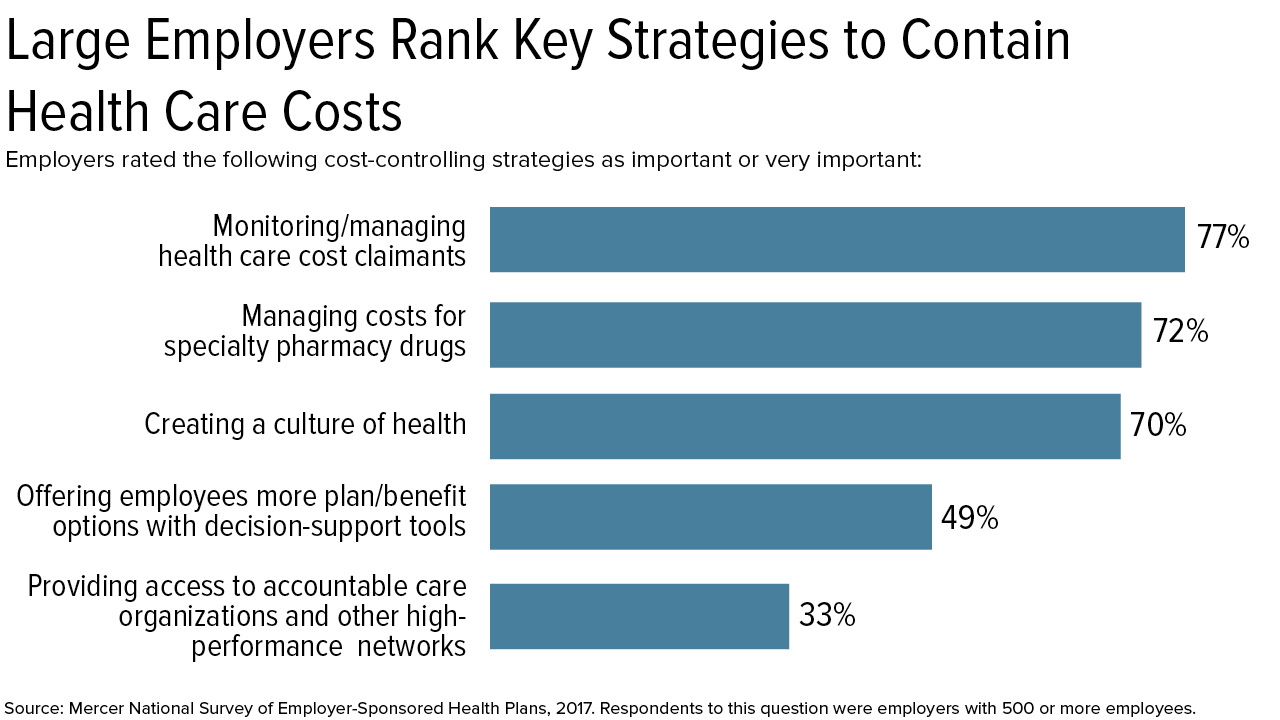
To keep health care expenses down and to improve workforce health, employers say they will manage and monitor employees who have made high-cost claims, a recent survey shows. More than 77 percent of U.S. employers with 500 or more employees said helping these claimants manage their care effectively was important or very important, according to analysis by HR consultancy Mercer in its National Survey of Employer-Sponsored Health Plans report, with responses from nearly 2,500 participating employers, polled last fall.
A rapidly growing share of health care claims is for services costing more than $50,000, Mercer found.
"High-cost claims are clearly one of the issues that keep employer health plan sponsors up at night," said Mercer's Jean Moore, senior director of health specialty practices. "Fortunately, there are ways employers can improve the experience of employees and family members dealing with serious conditions, while also mitigating cost. This can be done by helping to ensure that patients are receiving the right care, delivered in the right place at the right time."
Generally, a relatively small number of plan members drive a majority of the cost. According to Mercer's database of about 1.6 million plan members, the sickest 6 percent of an employer's population represents 47 percent of the total allowed medical and pharmacy spending, on average.
Personalized, "high-touch," nurse-centered care coordination can often improve health outcomes and cost efficiency, Moore said. An important difference between standard health advocacy programs and high-intensity care management programs, she explained, is that the care manager:
- Works directly with the care team as well as the patient and family.
- Stays in contact after hospital discharge to give support.
- Helps coordinate compliance with treatment plans.
According to a 2018 survey by Change Healthcare, a health benefits consultancy, employers are using several techniques to engage patients in their own wellness efforts. Results of the survey, conducted in late 2017 with responses from more than 2,000 of the firm's clients, show that the most frequent forms of intervention focused on providing access to:
- Wellness coaches (48 percent).
- Telehealth services (36 percent).
- Patient navigators trained to help small businesses and their employees evaluate health care marketplace coverage options and complete eligibility and enrollment forms (27 percent).
- Incentives awarded to members who display healthy behaviors (25 percent).
- Text messages, such as reminders to stay compliant with medications (12 percent).
[SHRM members-only toolkit: Designing and Managing Wellness Programs]
Cost Savings and Improved Health
"We can actuarially determine the savings and life-expectancy benefits individuals can achieve by effectively managing their health and making small behavioral changes," said Ron Mastrogiovanni, CEO of HealthyCapital, a provider of data and tools that encourage individuals to adopt healthy behaviors. "When employees are provided with personalized cost data related to something as important to them as health, they are more likely to take action."
A new white paper from the firm shows how savings from managing chronic conditions can motivate improved employee health and lead to lower costs for employers. Among the case studies it presents:
- A 50-year-old man diagnosed with high blood pressure and Type 2 diabetes would save around $2,000 per year in out-of-pocket health care costs before retirement and add three to eight years to his life expectancy by making a few behavior changes and taking prescribed medications.
- A 45-year-old woman diagnosed with Type 2 diabetes and high cholesterol could lower her annual out-of-pocket health care costs before retirement by more than $3,300—and add eight years to her life expectancy—by better managing her conditions.
Examples of positive behavioral changes include exercising moderately, eating healthfully and not smoking.
The findings underscore the savings possible through health condition management, Mastrogiovanni said. "Since employers pay, on average, around three-quarters of their employees' health premiums, the financial gains for self-insured employers [from improved employee health] are a multiple of the benefits for employees," he pointed out. "The lower expenses for employers offer opportunities to provide wellness support and financial incentives to further encourage healthier behaviors and savings."
Care Management's ROI
Recent studies delve further into the evidence for improved health outcomes and cost-savings return on investment (ROI) from providing chronic care management. A study published this month in Preventive Medicine found that population health-management efforts helped reduce heart attacks across a community of 4,000 adults in Minnesota. A study of carrier claims data from Mercer Health Advantage, a program offered through insurance carriers that features high-intensity care management for the sickest employees, showed an aggregate return on investment of $3.30 for each $1 spent while improving patient health.
The U.S. Centers for Disease Control and Prevention (CDC) population health tool, Healthy Days, measures physically and mentally "unhealthy days" on which individuals' activities are limited due to their condition. Health insurer Humana began collecting and linking healthy days data with health plan claims in 2014, with a total of 55,681 individuals included in its multiyear study. The findings, published last October in the American Journal of Managed Care and discussed in a 2018 Humana report, showed that each unhealthy day linked to a chronic condition costs health plans $15.64 in additional medical care per person, per month—a number that can add up quickly over time.
Not surprisingly, the study noted that patients with chronic conditions reported more physically and mentally unhealthy days than the population average. Patients who were compliant with certain quality measures related to chronic conditions, however, reported fewer unhealthy days than those who were not compliant.
Unhealthy days were "correlated with disease progression among our members who have diabetes, congestive heart failure and COPD [chronic obstructive pulmonary disease]," said Gil Haugh, director of Humana clinical analytics. The survey results "highlight the need to focus on both disease prevention as well as high-quality, integrated care delivery for patients who have been diagnosed with chronic conditions," he said.
Related SHRM Articles:
Rising Diabetes Rates Are Costly for Employers, SHRM Online Benefits, November 2017
Care Management Vital in Tackling Specialty Pharmacy Costs, SHRM Online Benefits, February 2017
Was this resource helpful?



